Monday, October 25, 2010
Recent 11th Circuit Opinion Regarding Iqbal Decision
The District Court dismissed his claims, citing Iqbal, but today the Eleventh Circuit issued a published decision reversing that dismissal. The Eleventh Circuit's decision emphasizes that every complaint must be read "as a whole" and construed in the plaintiff's favor, and that no plaintiff can be required to "prove his case on the pleadings."
Wednesday, October 20, 2010
ALLSTATE AGREES TO $10 MILLION REGULATORY SETTLEMENT OVER BODILY INJURY CLAIMS HANDLING PROCESSES
 Image via WikipediaAllstate has agreed to pay New York $1.2 million as part of a $10 million regulatory settlement, New York State Insurance Superintendent James J. Wrynn announced today. The agreement follows an 18-month targeted National Association of Insurance Commissioners (NAIC) multi-state market conduct examination of Allstate’s claims handling practices.
Image via WikipediaAllstate has agreed to pay New York $1.2 million as part of a $10 million regulatory settlement, New York State Insurance Superintendent James J. Wrynn announced today. The agreement follows an 18-month targeted National Association of Insurance Commissioners (NAIC) multi-state market conduct examination of Allstate’s claims handling practices. “Allstate has agreed to implement procedures to ensure transparency and fairness for consumers who have bodily injury claims,” Wrynn said. “The new processes ensure that claims will be handled consistently in different regions of the country, and consumers will have the right to get the information they need in order to understand how Allstate evaluates their claims and make sure they are fairly treated.”
The NAIC examination, for which New York was one of the lead states, focused primarily on Allstate’s use of claims handling software, particularly the software program, Colossus.
Colossus is a software program Allstate used to guide its settlement offers for bodily injury claims after automobile accidents. The examination found inconsistencies in Allstate’s management and oversight of the Colossus software program. In particular, the examination found that Allstate had failed to modify or “tune” the software in a uniform and consistent manner across its claims handling regions.
Under the settlement agreement, Allstate agreed to make a number of changes to its claims handling process, including:
- Providing notice to claimants that the Colossus software program may be used in the adjustment of their bodily injury claims;
- Enhancing its management oversight of Colossus to ensure that it adheres to established criteria and a uniform methodology in selecting claims to be used to “tune” or modify the software to reflect recently settled claims;
- Strengthening its internal auditing of Colossus and bodily injury claims handling to ensure adherence to written guidelines and procedures;
- Consolidating its bodily injury claims handling practices into a single claims handling manual; and
- Not establishing a policy or rule requiring claims adjusters to settle bodily injury claims solely on the value recommended by Colossus and not providing incentives for claims adjusters to settle claims at or near the value recommended by Colossus.
“It is important to note that we found no systemic underpayment of bodily injury claims,” Wrynn said. “While the issues addressed were serious, Allstate cooperated fully with our examination and is working to correct these deficiencies. Here in New York, we will continue to review the use of claims handling software by property/casualty companies.
“This settlement shows how state insurance regulators work together to protect consumers,” Wrynn said. “The four lead states – Florida, Illinois, Iowa and New York – worked cooperatively to conduct this examination and will keep working with the other 41 states that have signed on to this agreement to ensure it is fully implemented and consumers are properly protected.”
Allstate’s payment will be used to establish a regulatory fund. The fund will be used by the 45 signatory states, to the extent consistent with applicable state laws, to develop and train examiners to review and monitor the property/casualty industry’s use of software technology in adjusting claims.
Tuesday, October 12, 2010
11th Circuit Medicare Opinion Worth a Read
 Image by Kevandy via Flickr
Image by Kevandy via FlickrIn this very important decision, Bradley v. Sebelius, the 11th Circuit Court of Appeals approved a probate court’s equitable distribution findings to reduce a Medicare conditional payment obligation. Bradley, one of Charles Burke’s children and the P.R., brought suit against a nursing home for wrongful death as a result of nursing home abuse on behalf of the estate and ten surviving children.
Prior to Mr. Burke’s death, Medicare paid approximately $38k for his medical care in the hospital. The nursing home abuse case was settled for the entire amount of available insurance proceeds, $52, 500. A release was executed on behalf of the estate and the surviving children. Bradley notified Medicare of the settlement along with the procurement costs. Medicare refused to acknowledge that the claim had been settled for less than 100% of value. Medicare took the position it was entitled to the full amount of the medical expenses less procurement costs for a net amount of $22,480. Counsel for Bradley filed an application for the probate court to adjudicate the rights of the estate and rights of the surviving children in regard to the compromised sum received in settlement of the claims. Medicare was put on notice of the probate court proceedings and invited their participation in the proceedings. Medicare did not participate.
The state probate court ordered:
(c) . . . The Court after having heard sworn testimony on the potential value of each child/survivors’ independent claim, and after calling on its own experience in the range of values each child’s claim potentially carried, finds that the values asserted by the Personal Representative’s counsel in this motion are reasonable, and the Court adopts and specifically finds that each of the respective ten (10) survivors’ claims holds a value of at least $250,000.00. The Court notes that Medicare has asserted a claim of lien based upon payments of $38,875.08. Therefore, the Court finds that the total, full value of this case had the total, full value been collectible, was/is $2,538,875.08.
(d) Based upon principles of equity, the Court determines the medical expense recovery in the instant cause is $787.50. The Court has calculated such figure based on such component’s contribution to the total full value, if such value were collectible. The Court has not prioritized the recovery of medical expenses over the recovery on each of the respective survivors’ claims. Further, the Court determines the independent survivors’ claims recovery in the instant cause is $51,712.50. The Court has likewise calculated such figure based on all survivors’ claims contributions to the total, full value. The Court has likewise not prioritized the recovery on each of the respective survivors’ claims over the recovery of medical expenses.
Medicare refused to accept the probate court’s order that they would only recover $787.50. Based upon the Medicare Secondary Payer Manual, MEDICARE argued it didn’t have to recognize the probate court’s order since the order was not a decision on the merits of the controversy. Instead, the decision was an allocation of a settlement, not a judgment on the merits. See MSP Manual (CMS Pub. 100-05) Chapter 7, §50.4.4 (where “[t]he only situation in which Medicare recognizes allocations of liability payments to non-medical losses is when payment is based on a court order on the merits of the case”). Medicare argued that the probate court’s order was advisory in nature or superseded by federal law. Medicare was paid by Bradley under protest and an administrative appeal was pursued. All of Medicare’s administrative remedies were exhausted and Bradley lost at all levels. The case was appealed to federal district court for review of the Medicare administrative decisions.
The district court held that Medicare’s interpretation of the MSP, 42 U.S.C. §1395y(b)(2)(B)(ii)(2006), and its attending regulations, 42 C.F.R. §§ 411.37(c)(1),(c)(2), (c)(3)(2004), was reasonable. In making its decision, the district court relied heavily upon the Medicare Secondary Payer Manual, which does not recognize allocations of liability payments to non-medical losses unless it is an order on the merits of the case. The district court held Medicare was entitled to the entire conditional payment amount, less procurement costs, of $22,480. An appeal of that decision was taken to the 11th Circuit Court of Appeals.
The 11th Circuit examined the interplay between the Florida Wrongful Death Act (“FWDA”) and the MSP federal provisions. Bradley argued that the FWDA controlled. Under the FWDA, in a wrongful death action, survivors of the decedent may recover for lost parental companionship, instruction and guidance and for mental pain and suffering. Damages allowed to an estate are considered separate and distinct from damages recoverable by the decedent’s survivors according to Florida law. It is well accepted under Florida law that proceeds from a wrongful death action aren’t for the benefit of the estate, instead they are property of the survivors and compensation for their loss.
The court found that it was faced with an issue of first impression in this particular case and that was “[w]hose property is the settlement?” The court pointed out that the settlement involved medical expenses and costs recovered by the estate, subject to the MSP statute, along with non-medical, tort property claims of the surviving children for lost parental companionship under state law, not subject to the MSP statute. The Bradley court pointed out that all damages besides the decedent’s medical expenses where a property right belonging to the surviving children. Only the estate’s allocated share of the proceeds was subjected to Medicare’s claims.
The 11th Circuit was troubled by Medicare’s failure to participate in the probate court proceedings. Medicare declined to take part in the proceedings even though its position was adverse to the survivors in the proceedings. The court stated that “[c]ounsel properly turned to the Florida probate court for a proration, filing an application with the probate court to adjudicate the rights of the estate and rights of the children vis-à-vis the rights of the Secretary to the compromised sum received in settlement of the claims.” Yet even after the probate court made the allocation, Medicare asserted it was still entitled to the full amount less procurement costs based upon the MSP manual and refused to respect the decision of the probate court.
The court indicated that the essence of Medicare’s position was that the MSP manual was entitled to deference under Chevron, USA Inc. v. Natural Resource Defense Council, Inc. Under the Chevron Supreme Court decision, agency interpretation of a statute which it administers is entitled to deference. However, the Bradley court pointed out that the Supreme Court has held that “agency interpretations contained in policy statements, manuals, and enforcement guidelines are not entitled to the force of law.” The 11th Circuit concluded that Medicare’s reliance upon the MSP manual and the district court’s approval of such was misplaced.
The Bradley court correctly and aptly pointed out that that counsel for Bradley acted “sensibly” in settling the claim for the full value of all available insurance. If the MSP field manual was followed, it would lead to a “Catch-22” situation. It would force counsel to file a lawsuit inurring additional costs further diminishing the “paltry sum” available for settlement. According to the court, this would fly “in the face of judicial and public policy.” Therefore, the court held that Medicare’s position wasn’t supported by the statutory language of the MSP and its implementing regulations; the MSP manual does not control the law and it was error for the district court to rely “upon the advisory language contained in a field manual as the rationale for its opinion.”
Equally important, the 11th Circuit pointed out a second reason that Medicare’s position, as approved by the district court, was in error. The court reviewed the strong public policy favoring “expeditious resolution of lawsuits through settlement.” According to the Bradley court, Medicare’s position would have a “chilling effect on settlement.” This is so because Medicare’s position compels plaintiffs to force their tort claims to trial, burdening the court system. “It is a financial disincentive to accept otherwise reasonable settlement offers.”
For all of the foregoing reasons, the court held that Medicare was entitled to recover $787.50, as determined by the allocations of the state probate court. The Bradley opinion is a huge victory in the fight against Medicare conditional payment recovery in situations such as this. It is also is tremendously important because in the past the MSP manual has been treated deferentially, but not this time. Finally, it is important because it recognizes equitable distribution in the context of Medicare conditional payments and approves a state court’s allocation of damages in the context of a settlement. It should be a very useful case in fighting Medicare in the conditional payment realm.
Meridia Recall Diet/Obesity Drug by Abbott Laboratories
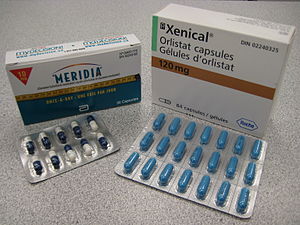 Image via WikipediaAbbott has issued a Meridia Recall after being asked by the FDA to stop marketing the product in the United States due to results of a study indicating an increased risk of heart attack and stroke in Meridia users.
Image via WikipediaAbbott has issued a Meridia Recall after being asked by the FDA to stop marketing the product in the United States due to results of a study indicating an increased risk of heart attack and stroke in Meridia users. Meridia (sibutramine) is a prescription weight loss drug marketed and sold in the United Stages by Abbott Laboratories, who have removed their Meridia webpage and issued a Meridia recall statement on their website.
According to Abbott, he FDA’s request for Abbott to remove Meridia from the US market is based primarily on the results of the SCOUT (Sibutramine Cardiovascular OUTcome Trial) study. This study researched about 10,000 patient, 6-year study requested by European regulatory authorities as a post-marketing commitment to evaluate cardiovascular safety in high-risk patients. Abbot maintains that most of these patients “had underlying cardiovascular disease and were not eligible to receive sibutramine under the current labeling“.
Patients should stop using Meridia (sibutramine) and consult their physician. Patients can also contact Abbott’s medical information line at: 1-866-257-8909.
Major banks forced to suspend foreclosures after 'robo-signing' of documents exposed
 Image by respres via FlickrGMAC Mortgage, JPMorgan Chase and Bank of America recently announced that they were suspending foreclosures after lawsuits exposed fraudulent practices. Other banks charged with illegalities include Wells Fargo, CitiMortgage, HSBC and National City.
Image by respres via FlickrGMAC Mortgage, JPMorgan Chase and Bank of America recently announced that they were suspending foreclosures after lawsuits exposed fraudulent practices. Other banks charged with illegalities include Wells Fargo, CitiMortgage, HSBC and National City.The Washington Post reported Oct. 9 that senior Obama administration officials were saying that "a nationwide moratorium on foreclosure sales may be inevitable, despite their grave reservations about the impact a broad freeze would have on the nation's housing market and economic recovery."
Problems turning up in courts across the country are varied, the New York Times reports, but all involve documents that must be submitted before foreclosures can proceed legally. Here are some of the more common shortcuts that have been exposed:
- Thousands of documents have been signed by employees, dubbed "robo-signers," who admit they have not verified crucial information like amounts owed by borrowers.
- Questionable legal notarization of documents has been common, in which, for example, the notarizations predate the actual preparation of documents—indicating that signatures were never actually reviewed by a notary.
- Other notarizations took place so far from where the documents were signed that it was highly unlikely that the notaries witnessed the signings, as the law requires.
- On other important documents, an official’s name is signed in radically different ways suggesting that some are forgeries.
This is a developing story that will have a wide and deep immpact




